Every American is acutely aware of the negative impact of drug and alcohol addiction; it’s impossible to ignore. Yet we have somehow missed a very positive story about addiction that is right in front of our nose. Tens of millions of our fellow citizens come out the other side to live substance-free, healthy and productive lives. It is a wake-up call to the reality of recovery in America, as well as a source of hope for the millions of American families who are currently struggling with drug and alcohol problems.
— Keith Humphreys, Professor of Psychiatry, Stanford University School of Medicine
Introduction
Conversely, those in recovery from drug and alcohol addiction are rarely the subject of media scrutiny or public attention. More than 22 million Americans, approximately, 1 in 10 adults, are in recovery, according to the most recent studies. Yet, the process of recovery, and those in recovery, are unlikely to be included in the public discussion about addiction.

Those in recovery, who accomplish milestones of sobriety and remission, are our friends, colleagues, and neighbors. Except for celebrities in recovery, ordinary Americans in recovery are not a media story or in the public realm. Their milestones of achievement in recovery are familiar only to their families and the recovery community, for example in AA and NA meetings when they receive chips for landmarks and touchstones in their sobriety.
Yet, referencing and acknowledging recovery is a necessary element of the discussion on alcohol and substance use disorders that is pertinent to individuals grappling with addiction, their loved ones, care providers, and healthcare policymakers. The flip side of addiction is recovery. A close analysis of recovery offers a blueprint for both those seeking remission from their addiction and those who treat them.
Definition of Recovery
The term “recovery” and the phrase “in recovery” have evolved over the last decade. In some quarters, both among those grappling with addiction, treatment professionals, and media, recovery from addiction is viewed similarly to recovery from illnesses such as the flu and other illnesses. In this context, recovery is seen as individuals who recover, or have recovered from or are recovering from addiction. The end result or recovery under this definition is total cessation of alcohol and substance use, and ultimate sobriety.
Over time, recovery’s definition evolved into one that centered on the longitudinal process and arc of recovering from addiction rather than a linear end result of abstinence and sobriety.
The new definitions of recovery that resonate with those who are grappling with addiction or have grappled with addiction in the past have holistic, comprehensive, global, overarching themes. It is as complicated and nuanced as alcohol and substance use disorders.

“Recovery from alcohol and drug problems is a process of change through which an individual achieves abstinence and improved health, wellness, and quality of life.”
Under the above definition, recovery is viewed as a quest for wholeness and a journey to individual self-actualization in every facet of one’s life—physically, mentally, emotionally, functionally, and practically. This state of being focused on personal wellness and one’s ability to function in every arena of one’s life as a result of abstinence.
Further refinement of this definition highlighted the idea of the individual’s relationship and responsibility to others. The result was a revision that highlighted external obligation and participation: “Recovery from substance dependence is a voluntarily maintained lifestyle characterized by sobriety, personal health, and citizenship.”
These formal and precise definitions though accurate and exemplary do not truly capture the meaning of recovery for those who are or were battling addiction. For them, recovery is a new lease on life, a total conversion from who they once were to who they are now, and who they hope to be. It is about living a full, happy, productive life in a community. Recovery for some of them is not abstinence from alcohol or substances but abstinence from destructive behaviors and actions that include alcohol and substances.

Recovery is a delicate process and journey with the ultimate goal of a fully resourced, good quality of life that includes all basic needs, and emotional and mental stability without the use of alcohol or substances. It is a closed-loop—not having an adequate quality of life can lead to a return to addiction; lack of abstinence can be an obstacle to acquiring basic needs and higher needs and achieving quality of life.
Seeking to engage in the process of recovery then is a decisive, aggressive act. It is a recognition that the life one is living is unfulfilling, unworthy, and untenable, and a declaration of intent to claim a life that is marked by all the features of self-actualization—emotional and physical wellbeing, enriching relationships with family and friends, participating in community and service, living up to one’s potential by pursuing education, vocation, and fulfilling work.
Road to Recovery
The Stages of Change and Recovery
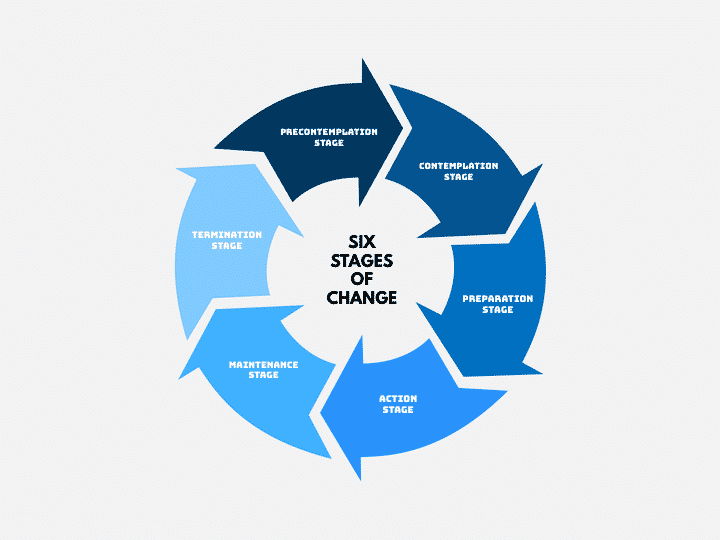
How people go through the recovery process is encapsulated in the “transtheoretical” model by Dr. Elizabeth Hartney which shows the stages of change that mark the recovery process. It is a logical yet unstructured process animated by the unique nature, motives, drives, and internal logic of individuals. Some may go through the stages in sequence, others may jump about, or double up on stages, or go backward. It is neither linear nor circular but a longitudinal journey through uncharted waters towards a promising beacon.
Pre-Contemplation Stage
At this early stage in the recovery process, people who are using alcohol or drugs do not meet the diagnostic definition of disorders or diseases. But they have awareness of their habit and may acknowledge to themselves that they have an unhealthy attachment to their choice substance. This may lead to a preliminary contemplation about giving it up. They’re usually of the opinion that their overuse of alcohol or drugs is a simple matter of exercising discipline and motivation. They may attempt self-detoxification and abstinence and relapse multiple times.
Contemplation Stage
The contemplation stage is usually kickstarted by a cataclysmic event—domestic violence, expulsion from school, termination from employment, abandonment by loved ones, drunk driving accidents that injure self or others, or kills; workplace accidents and crimes, arrest for possession or other crimes, a victim of crimes, or homelessness. The deliberate act to recover may be propelled by ultimatums by loved ones, compulsory court ordered rehabilitation as an alternative to imprisonment, or personal choice. At this stage, the addiction is already severe enough for individuals to consider treatment, though they may not rule out continued use. However, extending the metaphor of traveling through uncharted waters, it is the first sighting of land for those who understand that their addiction has overtaken their capacity to control it.
Preparation Stage
Action Stage
The individual determined to recover from his/her addiction is ready to act and claim sobriety as their right. This stage is tactical and demands the recovery seeker to activate all necessary actions in treatment that will lead to recovery. Many declare that this stage is the hardest part of recovery as it graduates from thinking about recovery and committing to recovery to actually doing everything it takes for recovery. It is the most exciting phase of recovery as it is done in the company of others—fellow recovery seekers, peer support groups, educators, therapists, counselors, and other healing modality practitioners. Recovery doesn’t happen in isolation but in fellowship and community.
Maintenance Stage
Termination Stage
At this stage in recovery, people find stability and grounding in their lives. After laying all the foundational stones for recovery, they are embedded on solid ground. They are emotionally and psychologically able to calculate the destructive consequences of relapse and reject a return to alcohol or drug use. They are able to discern triggers and cravings and steer clear of them and have the internal fortitude not to surrender to their worst impulses. In treatment, they will have received essential tools necessary to inoculate themselves against relapse.
Individuals at this stage are no longer the people they were during previous stages. They have recovered in every area of their life—health, relationships, careers, education, employment, finances, membership, and citizenship in the community.
The recovery community is a thriving, flourishing, nonjudgmental, forgiving one where people find camaraderie, community, understanding, and friendship.
Pathways to Recovery
In the cycle of recovery, the treatment phase is frequently an enriching, stimulating experience.
Those grappling with alcohol and substance abuse disorders routinely flourish and thrive as they submit to the recovery process in treatment.

When immersed in wraparound treatment and services, medication-assisted treatment, psychological and behavioral health modalities, therapeutic modalities, peer support, education, wholesome recreational activities; and nurtured by friendships forged through the common bond of addiction, the individual in recovery is able to reimagine, change, and reframe his/her relationship with alcohol and drugs. But leaving treatment elevates the avoidance of relapse into a battle for sobriety and survival.
People choose the pathway to recovery that meets their needs, that they can afford, and that aligns with their cultural and social fit. The pathways to recovery are either assisted or unassisted. Unassisted refers to self-driven recovery. Assisted, on the other hand, includes:
- Outpatient services
- Inpatient residential services,
- Peer support groups such as AA and NA
- Medication Dispensaries
- Community-based recovery services
- Faith-based recovery services
- Sober living environments
The most popular pathway to recovery are support groups such as AA and NA followed by outpatient treatment services including counseling and mental health.
Residential and outpatient treatment in clinical settings are veritable safe havens free from alcohol and drugs. Stripped from the family, community, and familiar culture and network of peers, co-users, enablers, and dealers with their own system of values, the recovering individual in treatment is able to imagine new possibilities.
Withdrawal, Abstinence, and Relapse
According to self-reporting, one of the reasons people continue to use alcohol and drugs and remain in addiction is because they are afraid of withdrawal symptoms.
By the time a person is fully committed to recovery, they have already tried to manage their addiction with frequent self-detoxification and abstinence without medical supervision. They inevitably return to using because of the effects of withdrawal.

Withdrawal symptoms from alcohol can be mild to severe depending on the severity of the addiction. The effects of withdrawal from highly addictive and potent opiates such as heroin and fentanyl can be excruciating. They include bone pain, stomach cramps, nausea, and diarrhea, profuse sweating, and shivering.
Without medical supervision and Medication-Assisted Treatment (MAT) to alleviate withdrawal symptoms, patients find it challenging to maintain abstinence and return to use and abuse. Methamphetamine, a fast-acting drug that delivers brief, intense bouts of euphoria, is a psychological addiction difficult to abstain from, that prevents people from committing to abstaining from it. Cocaine is a highly addictive social bonding drug that patients find difficult to abstain from. With its connotations of elitism, luxury, and partying, it is a frequent drug for those who relapse.
Medication-Assisted Treatment (MAT)
The latest treatment for alcohol and substance use disorders includes Medication-Assisted Treatment (MAT)—a disease management tool. It is an evolution in addiction science, a holistic treatment model component, and the gold standard in treatment for opioid use disorders. It allows patient stability through medication assistance and is a launchpad for recovery.
MAT is an evidence-based, next-generation addiction treatment that meets the most immediate and urgent needs of those suffering from opioid use disorders, by first allowing detoxification, and then stabilizing patients during transitory periods. An MAT protocol regulates brain chemistry and biological functions, relieves the symptoms of withdrawal from opioids, diminishes cravings, and improves a person’s ability to function normally.
A custom-designed treatment plan that includes MAT, psycho-social support, and behavioral health modules enable those who suffer from Opioid Use Disorders (OUD) to stay engaged in programs for the long term, significantly lowers a return to opioid use, increases immunity against relapse and overdose, and substantially increases the odds of sustained recovery.
When added to the arsenal of conventional treatment and wraparound support services, MAT is an exemplar in care for opioid use disorders. It has the capacity to address the chronic disease according to each patient’s needs. Several studies show that MAT reduces the likelihood of relapse and overdose fatality significantly.
The three FDA-approved MAT drugs for heroin and opioid dependency are Buprenorphine, Methadone, and Naltrexone.
Buprenorphine
A partial opioid agonist that at low to moderate rates mimics similar but low-grade effects of opioids such as euphoria or respiratory depression. It also blocks the effects of other substances. Since it’s a long-acting agent, it allows patients to have intervals in regimen. It diminishes withdrawal symptoms and cravings and lowers the risk of misuse and danger of overdose. It is prescribed as a tablet, cheek patch, or six-month implant under the skin at a doctor’s office after screening and evaluation.
Methadone
Naltrexone
MAT, when used as part of a customized full-spectrum treatment regimen that includes behavioral therapy and social support, offers the best outcomes for people suffering from opioid addiction. It is the gold standard in the arsenal of addiction treatment for those suffering from opioid and substance use disorders and has been shown to significantly reduce and prevent drug overdose deaths.
Medication-Assisted Treatment for opioid use disorders and addiction is an advance in modern medicine, akin to the advent of insulin in 1922 for the treatment of diabetes which was until then an untreatable, ultimately fatal disease. MAT and overdose reversal Naloxone is oriented towards addiction stabilization, disease management and life-saving. When combined with conventional wraparound services, they have the potential and power to significantly decrease the likelihood of relapse and the number of drug overdose deaths.
Recovery at New Leaf Detox & Treatment
At New Leaf Detox & Treatment, we are committed to meeting the needs of our patients with the most advanced best practices in addiction medicine and treatment and evidence-based standards of trauma-informed care, while always mindful of each client’s individual needs.
After the extensive patient-provider engagement, careful screening, and medical and psychological evaluation, our clinician’s design individualized plans to meet each patient’s specific needs. The plans are comprehensive in scope using a variety of treatment modalities from our cornucopia of specialized care plans that include Medication Assisted Treatment. New Leaf’s Medication Assisted Treatment plans for best client outcomes to feature three of the four FDA Approved MAT drugs: Buprenorphine, its extended-release injection Sublocade, and Naltrexone. These three MAT regimens and protocols have high success rates for clients when complemented with counseling and psychosocial support.
The patient begins cognitive-behavioral treatment with an individual therapist as well as in groups with a counselor to address the whole host of issues afflicting the patient, including anxiety disorders. Psychotherapy plans and specific treatment modalities tailored for the patient include individual counseling, group counseling, anxiety-focused therapy groups, and process groups and activities. The primary clinician and individual therapist and group counselor work in concert to treat the patient by resolving the underlying issues that led to addiction, followed by a variety of custom treatments that fortify the patient, clinical assessments throughout the process, and a considered discharge plan. Peer support, onsite medical assistance, family involvement, and post-treatment follow-up support are part of New Leaf’s standard of care.
Learn more here: nldetox.com For more information please contact us at 949-617-0719 or email us at info@nldetox.com
Conclusion
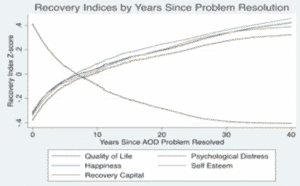
More than 22 million Americans are in various stages of recovery. They have used the array of existing pathways to recovery including support groups, counseling and other mental health modalities, inpatient treatment, outpatient treatment, Medication-Assisted Treatment, recovery community centers, and newer tools such as recovery and sobriety Apps. Remarkably and predictably, the positive quality of life for those in recovery increases over time while negative qualities diminish.

Longitudinally, over a period of three decades after addiction has been resolved, people’s happiness and quality of life rise on an upward trajectory, while negative qualities like psychological distress and low self esteem drop dramatically. As the field of Addiction Medicine matures, ever newer healing modalities will be available to help those committed to recovery to maintain recovery and stay in remission.
Recovery is everywhere. All across our country people are living healthy and productive lives in long-term recovery from addiction to alcohol and other drugs, benefiting themselves, their families and communities. Recovery is our best kept secret. It’s time to invest in understanding the solution to alcohol and other drug problems, advocate for the right resources to recover and demonstrate the power and proof of long-term recovery, offering hope to the over 23 million Americans who have yet to find recovery.
— Pat Taylor, Executive Director, Faces and Voices of Recovery
Sources
- Prevalence and pathways of recovery from drug and alcohol problems in the United States population: Implications for practice, research, and policy. (2017, December 1). ScienceDirect.
- Sticking with it: Predictors of continued medication use for opioid use disorder. (2021, August 27). Recovery Research Institute.
- National Recovery Study | Dr. John F. Kelly | Multiple Pathways to Recovery Conference 2017. (2018, May 21). Recovery Research Institute.
- Faces & Voices of Recovery.
- Recovery 101 – Information on Addiction Treatment and Recovery. (2021, August 25). Recovery Research Institute.
- Prevalence and pathways of recovery from drug and alcohol problems in the United States population: Implications for practice, research, and policy. (2018, December 1). National Center for Biotechnology Information.
- Treatment and Recovery. (2020, July 10). National Institute on Drug Abuse.
- Psycom.net. (2021, June 28). Addiction Recovery: Reasons to Recover from a Girl Who’s Been There. Psycom.Net – Mental Health Treatment Resource Since 1996.
- The Five Rules of Recovery and Relapse Prevention. (2017, December 1). Addictions and Recovery.
- Addiction and Recovery | Kaiser Permanente.
- Putting text message post-treatment follow-up interventions to the test. (2021, August 27). Recovery Research Institute.