Although about 21 million Americans struggle with addiction, only about 10% reach out for help.
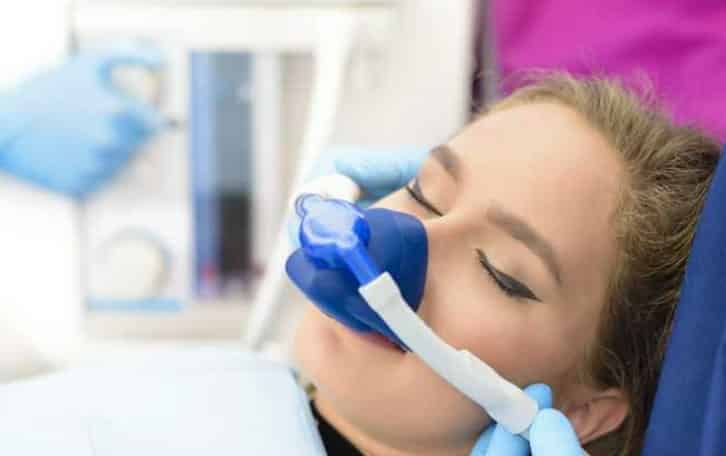
Finding help can be intimidating and overwhelming. If you or your loved ones are trying to detox from heroin or any opioid, it’s easy to try to reach for a quick fix like a rapid, sedation detox. On paper it sounds great: a detox method completed entirely while sedated and asleep.
Sedated detox is marketed as a silver bullet for addiction, but it presents severe risks and complications. Before undergoing any medical procedure it’s important to fully understand the risks. In this article, we will go over the risks and benefits of rapid medical detox, and how to form a comprehensive treatment program.
What Is a Sedation Detox?
Sedated detox is also known as Anesthesia-Assisted Rapid Opiate Detoxification (AAROD). It is promoted as one of the quickest ways to go through withdrawal.
In AAROD, doctors place the patient under general anesthesia and administer opiate antagonists. The medications are intended to flush out active opiates from the patient. This step replaces the withdrawal phase in typical recovery programs.
After the anesthesia phase, treatment continues with the medication Naltrexone. Naltrexone blocks the effects of opiates by attaching itself to receptor sites. Blocking the receptors means that the patient cannot get high. The patient continues the Naltrexone program for about six months to a year.
AAROD is an effective detox for addicts who are physically addicted to opiates such as Heroin or Methadone. The FDA has approved all drugs used in AAROD.
Benefits of AAROD
Because of the rapid withdrawal period, AAROD is a quick substitute for traditional withdrawal. It replaces the usual week of withdrawal symptoms with 3-5 hours of anesthetized withdrawal.
Although many users experience residual withdrawal symptoms, they fade over time. The patient completes most of the withdrawal process while asleep. The patient, therefore, requires a shorter hospital stay before they are released to counselors or family.
Effectiveness
Alone, AAROD is no more effective than a traditional withdrawal. A recent study performed by the College of Physicians and Surgeons of Columbia University found that AAROD was not an improvement over traditional detox programs.
A follow-up study at Columbia University Medical Center compared rapid detox with two other detox methods. The patients who underwent AAROD experienced similar discomfort levels to the other two methods. They also experienced more serious side effects. The results found that the outcomes were very similar.
While AAROD is still effective, it is comparable to other methods that are safer and less expensive.
Likelihood to Relapse
Detox is only the first step. Patients require continued treatment to prevent a relapse. Both AAROD and traditional detox also require additional treatment plans. Treatment plans can include a residential stay or outpatient services.
A rapid detox program doesn’t address the fundamental causes of drug dependence. Furthermore, it can’t replace drugs with healthy coping mechanisms. Consistent psychotherapy allows patients to address the causes of their addiction. Treating the causes helps prevent relapse.
The science is clear that those who choose AA or other psychotherapy are more likely to experience remission and avoid relapse. A therapy routine should follow any detox method to prevent relapse and fully recover from addiction.
Risks and Complications
AAROD cleanses the body of opioids so quickly that it can be a significant shock to the system. Although the procedure takes place under medical supervision in a hospital setting, AAROD is still considered dangerous and can have significant side effects including death.
Because it is so risky and the benefits are slim, the American Society of Addiction Medicine does not recommend the AAROD for treatment.
Worsening Mental Health
Drug abuse is a serious mental illness that is often brought on by a separate mental illness as a coping method. In many cases, opiates provide relief from mental health symptoms. If the patient withdraws from opiates without replacing them with healthy coping strategies, they are in danger of worsening mental health.
Recovering from mental illness requires therapy and counseling to manage symptoms. If patients were magically cured of their drug dependencies, they’d still confront a mental illness that hasn’t been properly treated. Undergoing AAROD risks letting an underlying mental illness run rampant.
Mental health risks underscore the need for residential treatment or structured outpatient treatment. It’s not enough to just remove the drugs from the body; Both the body and mind need treatment.
Death and Serious Complications
The CDC discusses an event in which a pattern of severe effects of AAROD was revealed. In 2012, the Department of Health was notified that many patients who had undergone AAROD faced serious reactions. Out of 75 patients, five required hospitalization, and two others died.
One of the patients manifested panic attacks and violent behavior. They were then admitted to the emergency room with suicidal thoughts. The patient was ultimately successfully treated. This is a concrete example of how simply treating addiction with AAROD can expose an underlying mental illness.
Two other patients experienced pulmonary edema while two others experienced cardiac arrest. One of the cardiac events was fatal. The remaining patients experienced sepsis, electrolyte imbalances, or a fatal brain stem herniation.
In other studies of AAROD, some percentage of patients also experienced life-threatening events.
Ready to Get Help?
Despite the marketing of sedated detox, there’s no quick fix for addiction. But, that doesn’t mean that there’s no hope. Help is always available to those who ask for it.
Don’t substitute treatment with medication, and don’t sleep through the process. Instead, take an active role in your recovery and opt for a safe, holistic approach. New Leaf, in San Juan Capistrano, offers comprehensive care, safe detox, and mental and physical treatment. Reach out today to discuss treatment options.