“Everybody has to learn their relationship with alcohol and drugs… No one can get sober for their jobs, for their wife, for their kids. They can’t do any of that. They could only do it when they decide they’re done, truthfully… When the light goes on there’s hope.”
- Rob Lowe on The Kelly Clarkson Show
Disclaimer: Only for fair use for educational purposes and illustration. We do not own the copyright to this video.
Decades of scientific research have settled the fact that alcohol and substance use disorders are chronic neurological diseases complicated by an array of individual experiences and vulnerabilities; communal, cultural, and societal influences; and genetics and family history. Yet personal responsibility and commitment are viewed as essential to recovery.
Overcoming an addiction to alcohol and substances then requires both the management of a chronic disease, and the use of behavioral and psychological tools and social support to progress through recovery. For those who see themselves as mere mortals, who are powerless against uncontrollable urges to consume the drug of their choice, they cannot imagine mustering the strength and will to succeed. For many, recovery and sobriety seem unreachable, elusive, and unattainable. It is an arduous journey, the work of a lifetime, that demands so much from addicted individuals.
But the journey through recovery and sobriety begins with only two steps—an authentic intention to cease using alcohol and substances, and a personal commitment to maintain recovery and beat the addiction. The overarching goal, organizing principle, and bold vision of a life without alcohol or substances serve as powerful motivators and propulsive forces to keep going no matter what—despite setbacks, obstacles, challenges, and relapses. Keeping one’s eyes on the prize—a rewarding life sustained without alcohol or substances—helps those in recovery manage their illness and maintain sobriety, as they continue to create a self-actualized life beyond their expectations, using their talents and newly developed skills.
The road to recovery is a difficult one that demands faith in one’s ability to change, hope and optimism in the process, discipline in submitting to the process, and courage to stay the course. But despite the hardships, the road to recovery, to turn over a new leaf, is worth taking because the alternative either diminishes the quality of one’s life, robs it of meaning, or endangers it altogether.

The idea of change is frightening to most people. When faced with a call to change, most people’s initial reaction, often visceral or reflexive, is to resist.
“I am what I am. Take me as I am. I will not change,” is usually the immediate reaction among hardened, well-defended individuals.
Others may consider change because they recognize the validity of the call to change—for example, when someone important to them calls out the impact of their behavior on others. Some may consider change if they see benefits for changing—for example, the potential for a job promotion or salary increase.
Still, others will be forced to consider change in the face of pain caused by alcohol or substance abuse. Those in danger of losing careers, or marriages, or child custody, and those facing civil liability or criminal penalties including imprisonment as a result of their alcohol or substance abuse will be compelled to change.
It is the beginning of recovery, one immortalized as the First Step in Alcoholics Anonymous. “We admitted we were powerless over alcohol and that our lives had become unmanageable.”
Inaccurate science about the theory of change also frightens many. For nearly five decades, self-help gurus have popularized and misrepresented a notion first offered by Dr. Maxwell Maltz, a cosmetic surgeon who authored a bestselling self-help book, Psycho-Cybernetics. Maltz ventured that in his practice, he observed that his patients took approximately 21 days to get accustomed to their post-surgical appearance. He also noted that amputees under his care overcame “phantom limb syndrome” (the phenomena of awareness and feeling of limbs despite amputation) after about 21 days.
Since his declaration in 1960, a legion of self-help gurus have misinterpreted his personal, non-scientific observation to posit categorically that changing a habit takes 21 days.
The “21 days to change” myth has been perpetuated in the culture, as well as by motivational speakers and alternative healthcare treatment providers, resulting in expectations by those seeking treatment for alcohol and substance addiction and their loved ones. This false notion sets up those seeking treatment for failure and imbues them with a sense of failure. As well, families of those in recovery feel disappointment or anger towards their addicted loved for their lack of progress or relapse.
In addition to understanding the fundamental nature of Alcohol and Substance Abuse disorders—that they are chronic neurological diseases that must be managed throughout a lifetime—it is essential to understand the brain’s role in habit forming and addiction.
Habits and addictions are resistant to voluntary change and require a whole arsenal of tools, treatment, and therapies to support gradual habit-breaking that leads to transformational change. Understanding the workings and architecture of the brain, its role in addiction, and the elements of addiction treatment, will allow those grappling with alcohol and substance abuse disorders to grasp and prepare for the challenges and pitfalls in treatment and recovery. Knowing the power and limits of the brain will help them through recovery and understand relapse and recurrence.

Individually and in unison, neurons and neural networks transmit signals to perform these and other diverse and specific functions.
Chemical agents serve as neurotransmitters to relay the transmission of signals. They infuse the gaps between cells and bridge the gaps to send signals from cell to cell. The resulting communication enables functionality and performance. The chemicals transmit from neurons through synapses to receptive neurons, and cascade and surge through the body during specific events, times, and experiences to address precise needs.
In the healthy brain, the alchemy of chemical and electrical processes work alone or in concert to control basic functions. Each type of neurotransmitter has distinct qualities and functions; some inhibit action, others stimulate activity. Some are responsible for basic functions such as breathing and digestion, others for higher functions such as thinking, emotions, learning, and memory. Some communicate exclusively with muscles to stimulate physical action, still, others influence a person’s reactions to external events including sounds, smells, and a myriad of sensory stimuli.
Hundreds of chemicals, a veritable pharmacy, inhabit our brain allowing it the ability to orchestrate the body to function and maintain homeostasis and equilibrium. The five major chemical neurotransmitters are: serontonin, oxytocin, dopamine, norepinephrine, and Gamma-aminobutyric acid aka GABA.
Understanding what each neurotransmitter does in the healthy brain also informs how it reacts in the addicted brain.
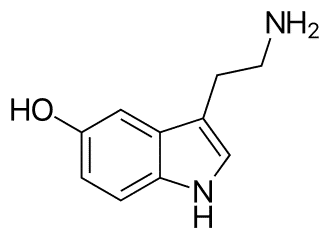
Serotonin regulates sleep and emotions, influences sexual desire and arousal, impacts appetite and digestion, and powers motor and cognitive actions. It promotes happiness and positive feelings.
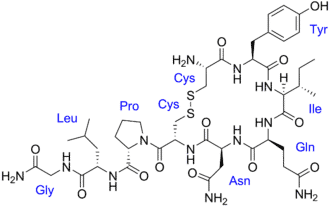
Oxytocin is requently referred to as the “love” chemical because of its critical role in human relationships, social behavior, and intimacy. It is instrumental in relationship building and sexual, romantic, and familial bonding. Mothers in labor and during breastfeeding release Oxytocin, as do lovers.
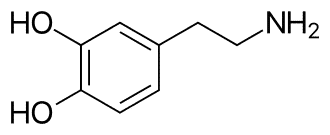
Dopamine is the neurotransmitter that gives us our mojo to focus and strive and find meaning and pleasure in our lives. It allows us to be strategic beings who think, learn, strive, ruminate, consider, and plan. It also regulates heart rate, sleep, mood, and pain.

Norepinephrine is released in the body during stress and trauma, calming the nerves and making people alert, aroused, and nimble to address the stress-inducing event. It elevates focus and concentration and has a positive effect on mood. Deficits in this neurotransmitter can cause Depression and ADHD.

Gamma-Aminobutyric Acid (GABA) is a subduing neurotransmitter that inhibits or blocks activity in the brain and nervous system. The release of GABA calms negative moods, relieves anxiety and pain, improves sleep, and lowers hypertension. It also boosts the benefits of exercise by burning fat and increasing lean muscle growth.
The basal ganglia, prefrontal cortex, and extended amygdala serve important functions in humans.
The basal ganglia is the reward and pleasure center of the brain. A rush of chemicals surge through the basal ganglia during pleasurable events, such as eating delicious food or having sex, or when thrilled by an experience or activity.
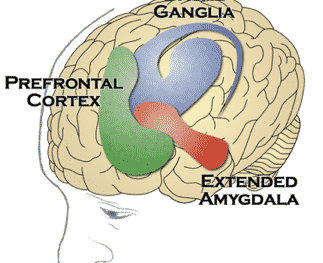
The urge to repeat the pleasurable experience is inevitable. This region of the brain is naturally activated to feel pleasure when consuming drugs or alcohol. Habit forming and addiction gradually occur when we seek to relive the euphoria of our substance.
The extended amygdala which activates the survival instinct in the face of anxiety, stress, fear and danger is compromised and even hijacked by substance abuse and withdrawal.
The prefrontal cortex which is responsible for higher thinking, judgement, and executive function that allow people to organize priorities, strategize plans, and design actions, can be either deployed in the service of consuming substances or damaged by repeated use.
Drugs and alcohol take a toll on the brain. Some have wide-ranging effects on a whole symphony of neural activity, while others may affect just one neurotransmitter. Alcohol increases serotonin levels in the brain, while cocaine increases dopamine activity resulting in euphoria. Heroin and prescription opioids resemble naturally occurring chemicals in the brain such as endorphins, but are turbo-charged versions that decrease pain and focus, and slow respiration at a greater rate.
Drugs can disrupt one neurotransmitter while creating a cascading effect on other neurotransmitters by simulating the properties of naturally occurring chemicals in the brain. Both marijuana and nicotine attach to receptors and mimic neurotransmitters. Benzodiazepines alter the regular process of neurotransmitters to elicit relaxation. Some drugs are dangerous and toxic to neurons. For example, MDMA/Ecstasy/Molly damages serotonin delivering neurons to wipe out memory and recall. Meth use affects dopamine-releasing neurons and damage thinking and motor skills.
The physical structure of neurons may also change with repeated use of substances. Repeated and extended use of alcohol and drugs wreak havoc on naturally occurring neurotransmitters, provoke a surge of neurotransmitters in abnormal quantities, and creates abnormal neural communication.
Drugs and alcohol become more satisfying than natural rewards which make normal life and activities colorless and joyless. Dopamine surges caused by repeated ingestion of substances give intense, prolonged “highs” that are rarely replicated by normal activities. This creates a strong desire for substances for more and more “highs” and reinforces the need for more substances. Absent the alcohol or substance, cues around us that are associated with drug use, such as certain friends who are our drug buddies, or concerts, can trigger uncontrollable urges and cravings for our drug of choice.
At some point, the user needs more and more amounts of their preferred drug to recapture the intensity of previous highs, because they have built a tolerance. The user gets trapped in a vicious cycle of addiction of highs and lows, all the while wrecking their physical and mental health in ever-increasing increments.
To read more about the brain and addiction, please see our article, Relapse and Recovery.
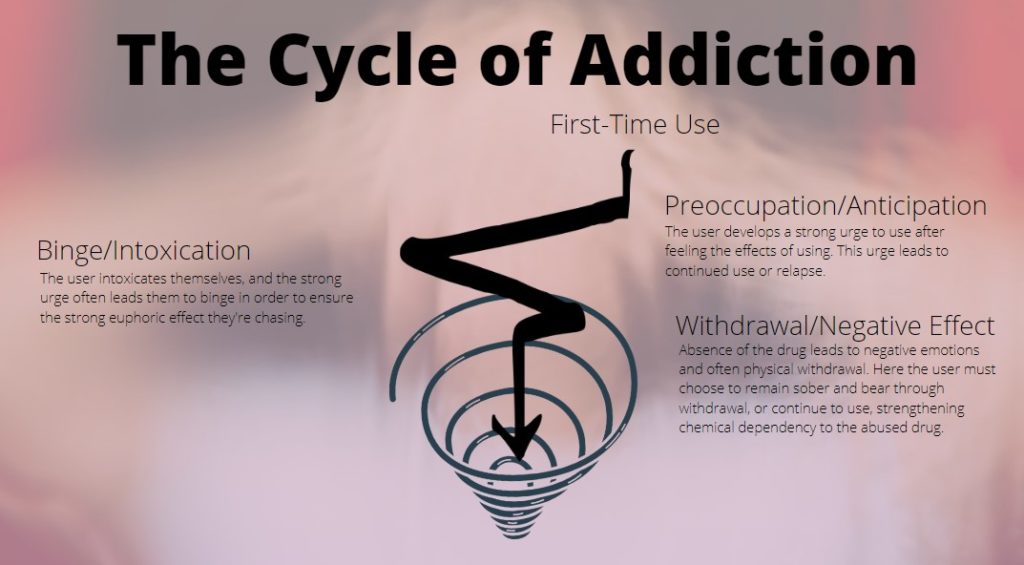
There are a quartet of behaviors that are evident in those suffering from alcohol and substance abuse disorders. The four behaviors take a central role in every phase of the addiction cycle. They are impulsivity, positive reinforcement, negative reinforcement, and compulsivity.
Alcohol and substance abuse creates a rollercoaster of emotions that range from depression and futility to numbness and euphoria.
As the user is depleted physically and mentally with only occasional bouts of positive feelings after ingestion, the individual may contemplate, or be forced to contemplate, treatment, recovery, and sobriety. At this point, the person is suffering from a medical emergency marked by clinically serious mental, physical, and emotional deterioration.
At New Leaf Detox and Treatment in San Juan Capistrano, we are acutely sensitive to the individuality of each client who walks through our doors. New Leaf Detox & Treatment offers the gold standard of care in rehab—residential detox and treatment. As a best practice, it views the journey of addiction recovery and sobriety through a trauma-informed lens. New Leaf maintains that a holistic approach to recovery and sobriety can only be addressed through trauma-informed care. The entire clinical and support staff here are trained in trauma-informed care.
Once an individual commits to, and invests, in his or her recovery, the team at New Leaf embraces the patient’s efforts and activates the goal of recovery and sobriety with trauma-informed sensitivity and care. A primary clinician at New Leaf engages with the patient and does a number of evaluations and screenings, trauma included. Directed by the primary clinician, the patient begins detox with or without medication-assisted treatment. The levels of care offered at this industry-leading rehab include Detox, Inpatient Rehab, and Dual Diagnosis. More details here.
New Leaf’s substance-specific programs have treated clients from around the nation. They include specialized care and treatment for addictions to alcohol, heroin, cocaine, marijuana, stimulants, benzodiazepine, and prescription drugs. More details here.
We customize treatment plans by clinically curating from a roster of the most successful evidence-based modalities that treat every aspect of a person’s case, body, mind, and spirit. These include:
Medication-Assisted Treatment, Trauma-Informed Care, Cognitive Behavioral Therapy, Holistic and Yoga Therapy, Physical Recovery, and Psychotherapy. More details here.
We view sobriety and recovery as a process of change and transformation. Our name, New Leaf, is a metaphor for the change and transformation that begins for our clients when they commit to walking through our doors, and for our commitment to helping them turn over a new leaf, in all the ways we can.
The most critical factor in your recovery and sobriety is the person you see in the mirror. Without the intention and active commitment of the person in the mirror, her/his hopes for recovery and sobriety will not be realized. The only person who can make a claim to recovery and sobriety is the person who commits to it. It is a commitment to one’s own worth as a human being, to one’s dreams for a future filled with potential.
The intention and commitment you make to your own recovery is a declaration that you are worthy, that you deserve a life worth living. The declaration will strengthen you and carry you through difficult days, through days when you wish to score drugs to alleviate your pain, through doubts, through pain, through failure, and even through relapse. It is essential to your success, critical to your life. All you need to commit to is to be sober just for today. Then renew your commitment the next day and the next. It adds up to a lifetime. One day at a time.
U.S. Department of Health and Human Services (HHS), Office of the Surgeon General, Facing Addiction in America: The Surgeon General’s Report on Alcohol, Drugs, and Health. Washington, DC: HHS, November 2016.
NIDA. 2020, July 10. Treatment and Recovery. Retrieved from https://www.drugabuse.gov/publications/drugs-brains-behavior-science-addiction/treatment-recovery on 2021, February 22
Centers for Disease Control and Prevention, National Center for Injury Prevention and Control. (2020, August 12). Recovery Is Possible. Retrieved February 22, 2021, from https://www.cdc.gov/rxawareness/treatment/index.html
The Centers for Disease Control and Prevention. (n.d.). Addressing the Prescription Opioid Crisis: CDC Rx Campaign Overview. Retrieved February 22, 2021, from https://www.cdc.gov/rxawareness/pdf/Overview-Rx-Awareness-Resources.pdf
Figee M, Pattij T, Willuhn I, Luigjes J, van den Brink W, Goudriaan A, Potenza MN, Robbins TW, Denys D. Compulsivity in obsessive-compulsive disorder and addictions. Eur Neuropsychopharmacol. 2016 May;26(5):856-68. doi: 10.1016/j.euroneuro.2015.12.003. Epub 2015 Dec 11. PMID: 26774279.
National Institute on Alcohol Abuse and Alcoholism. (n.d.). Alcohol’s Effects on Health. Retrieved February 22, 2021, from https://www.niaaa.nih.gov/alcohols-effects-health
NIDA. 2020, July 10. Drugs and the Brain. Retrieved from https://www.drugabuse.gov/publications/drugs-brains-behavior-science-addiction/drugs-brain on 2021, February 22
Substance Abuse and Mental Health Services Administration. (2020, April 23). Recovery and Recovery Support. Retrieved February 22, 2021, from https://www.samhsa.gov/find-help/recovery
American Society of Addiction Medicine. (2014, June 12). On Impulsivity: The Neuroscience of Behavior Associated with Addiction. Retrieved February 22, 2021, from https://www.asam.org/Quality-Science/publications/magazine/read/article/2014/06/12/on-impulsivity-the-neuroscience-of-behavior-associated-with-addiction
Columbia University Irving Medical Center. (2018, February 20). The Science Behind Behavior Change. Retrieved from https://www.cuimc.columbia.edu/news/science-behind-behavior-change
Hill, T. (2019, March 25). Is Addiction a Choice? Retrieved from https://www.mentalhealthfirstaid.org/external/2019/03/is-addiction-a-choice/
New Leaf Detox and Treatment
63 Mallorca, Laguna Niguel,
CA, 92677
(844) 929-0067